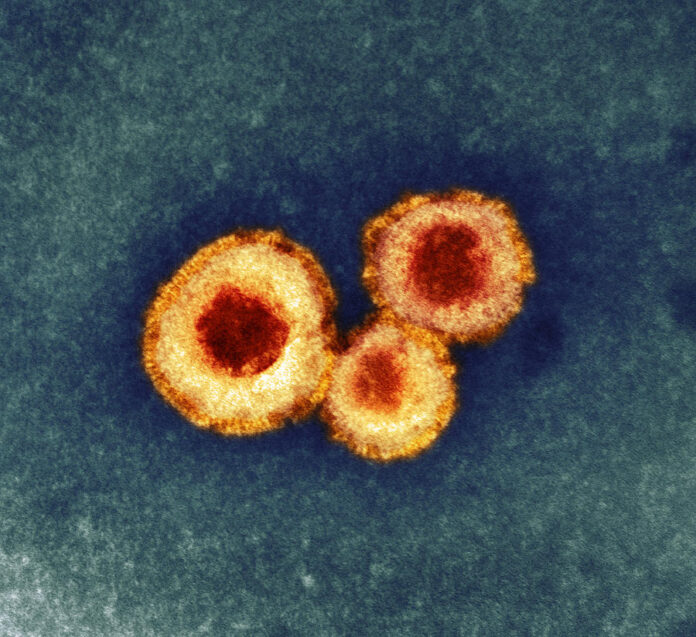
TARLAKENYO (June 10, 2023) — A recent report released by the Centers for Disease Control and Prevention (CDC) indicated an increase in human metapneumovirus (HMPV) cases.
Respiratory tract infections, which are a common occurrence worldwide and a major cause of illness and death, continued to be prevalent during the recent cold and flu season.
As people began to reduce mask usage and interact more frequently with individuals outside their households, there was a notable rise in respiratory syncytial virus (RSV), influenza, and COVID-19 cases. However, just as the frequency of these cold and flu viruses was declining, the CDC identified a surge in HMPV cases.
In mid-March, the virus reached its peak, with nearly 11% of PCR tests returning positive results.
Before the pandemic, the number of positive HMPV cases remained around 7%. However, experts in infectious diseases believe that the over 35% increase in cases is largely due to the population’s limited immunity against the virus.
According to Dele Ogunseitan, Ph.D., MPH, an infectious disease specialist and professor at the University of California, Irvine, most parts of the world experienced a period of hibernation or lockdown for the past two years, resulting in a lack of circulation of these viruses among the population.
As a result, people did not develop the natural immunity that would have provided some protection against HMPV infection. When individuals recently started to socialize and travel more, these infections experienced a surge in transmission.
What is Human Metapneumovirus?
HMPV is a well-known virus that has been present since at least 2001, and it potentially existed even earlier. In healthy individuals, it usually causes mild symptoms similar to a common cold, but it can become more severe.
HMPV is closely related to avian metapneumovirus, suggesting that it may have originated from birds and subsequently crossed over to humans or vice versa over 75 years ago. The virus primarily affects the lower respiratory tract and is the second most prevalent virus after RSV.
Research indicates that nearly all children contract HMPV by the age of 5, but because complete immunity is not achieved, reinfections can occur throughout adulthood.
While HMPV has been circulating in humans for decades, it remains relatively unknown to the general public, as it is not routinely tested for.
Brian Labus, an infectious disease expert, explains that HMPV is a common cause of illness during colder months, often circulating alongside other cold and flu viruses.
Labus suggests that the COVID-19 pandemic may have affected the community’s level of immunity to HMPV due to reduced exposure over the past couple of years.
Symptoms of Metapneumovirus
HMPV commonly presents with symptoms similar to a cold, such as cough, sore throat, fever, runny nose, and nasal congestion. While some individuals may be asymptomatic, others can experience more severe manifestations, including wheezing, difficulty breathing, and even hypoxia, which may require hospitalization.
HMPV, like other cold viruses, spreads through respiratory secretions released during coughing and sneezing.
It can also be transmitted by touching the eyes, nose, or mouth after coming into contact with contaminated surfaces.
In most cases, HMPV infections resolve on their own within a few days without specific treatment.
However, certain individuals, such as infants, young children, older adults, and those with weakened immune systems, are at a higher risk of developing severe respiratory illnesses like bronchiolitis and pneumonia due to HMPV infection.
The incubation period for HMPV is estimated to be approximately four to six days, although some studies have detected viral RNA up to two weeks after symptom onset. Typically, most individuals recover from HMPV infection within about seven days without requiring specific treatment.
Unfortunately, there are currently no FDA-approved antiviral medications or vaccines available to treat HMPV, highlighting the need for preventive measures and supportive care to manage the infection.
Should we be concerned?
While HMPV infections are typically mild and resolve on their own, it is important to be cautious, particularly in children, older individuals, and those with weakened immune systems, as they are more susceptible to complications, as cautioned by Dele Ogunseitan.
Moreover, co-infections of HMPV with other viruses can exacerbate the severity of the illness and even lead to severe complications and death.
Studies have shown that a significant portion of hospitalized individuals with HMPV and another virus were at least 65 years old, with a high mortality rate reported in long-term care facilities due to the development of bronchitis or pneumonia.
Children between 6 and 12 months of age are particularly vulnerable to hospitalization from HMPV, which differs from the peak age of hospitalization for RSV occurring around 2 to 3 months of age.
Alarming statistics reveal that millions of HMPV infections occurred in children under the age of 5 in 2018, resulting in a substantial number of deaths.
If symptoms persist for more than seven days or if there are specific risk factors such as age over 60, infancy, or underlying medical conditions, it is crucial to seek evaluation from a healthcare provider. Immediate medical attention should be sought if wheezing or breathing difficulties are experienced.